-
Endometriosis is commonly associated with infertility. About half a million Australian women are suffering from endometriosis, with an increased likelihood in their 20s and 30s. Endometriosis is a condition in which tissue-like endometrium (lining the uterus) grows on surrounding pelvic organs. While many women with endometriosis can have children without difficulty - 30% of women with endometriosis have trouble with fertility and difficulty falling pregnant.
Here, I will answer some common questions about the link between endometriosis and fertility and how it can affect pregnancy.
Is there a link between endometriosis and fertility?
Endometriosis can affect fertility in different ways - it can distort pelvic anatomy by forming scar tissue in and around the tubes and ovaries. This can affect egg pick up by the tube, the movement of sperm, egg fertilisation, embryo growth and implantation. Endometriosis is also associated with poor egg quality.
Endometriosis contributes to 30% of women who are having difficulty to conceive. Some women with endometriosis feel pressured to have children as soon as possible to increase their chances of becoming pregnant. Others may be ready but unable to fall pregnant, resulting in frustration and hopelessness which can, in some cases, lead to depression. Diagnosis of endometriosis is often made as part of investigations of infertility. This may add further distress over trying to fall pregnant.
What effect can endometriosis have on a pregnancy?
Until now, pregnancy risks in women with endometriosis were unknown. New research findings1 have shown that pregnant women with endometriosis are at higher risk of both early and late complications in pregnancy and need close antenatal monitoring.
Endometriosis increases the risk of miscarriage and ectopic pregnancy, has higher preterm birth rates and caesarean section births.
Read more about the effect of endometriosis on pregnancy
What effect can pregnancy have on endometriosis?
Symptoms of endometriosis may improve during pregnancy due to high progesterone levels. The effects of endometriosis after delivery are unclear and recurrence can happen.
How is mild endometriosis associated with infertility treated?
Endometriosis associated with infertility can only treated with surgery. The aim of surgery is to reduce symptoms and improve fertility by removing endometriosis lesions, nodules and pelvic adhesions to restore reproductive anatomy. Surgical treatment to improve the fertility is the most effective for minimal to mild endometriosis.
If surgery is unsuccessful, in vitro fertilisation (IVF) may also be considered. It is important that endometriosis is properly treated prior to IVF as the treatment increases oestrogen levels and can encourage the growth of existing endometriosis. Medication to suppress ovarian function does not improve infertility and it should not be offered.
How is severe endometriosis associated with infertility treated?
The lack of consensus about fertility treatment for women with stage III or IV endometriosis is due to limited evidence-based data. However, have shown that surgical treatment of severe endometriosis does improve spontaneous pregnancy rates of 52–68%, versus 0% after expectant management. Multiple studies of IVF for women with severe endometriosis show conflicting results, but generally, success rates depend on the age (under 40) and number of eggs collected during the ovarian stimulation.
What is endometrioma and is it linked to infertility?
This is one of the controversial issues regarding endometriosis among infertility specialists.
Endometrioma is a cyst formed when endometriosis tissue grows in the ovaries. Endometriomas can associated with reduced fertility, although a direct causal relationship has not been well established. Removal of ovarian endometrioma above 3 cm has been associated with improvement of spontaneous pregnancy. But, evidence of the impact of endometrioma on ovarian response during IVF is equivocal. Repeated or extensive ovarian surgery should be avoided as it can have a detrimental impact on ovarian reserve. The theoretical benefit of performing surgery to improve pelvic anatomy and accessibility has not been supported with clinical evidence. Many uncertainties remain on the optimal treatment of an endometrioma, hence the decisions should be individualised based on women’s choice, age, ovarian reserve and associated symptoms.
Getting help
The take home message for treatment for endometriosis associated with infertility is that your doctor will need to tailor your treatment plan to your individual needs. This is because treatment decisions depend on factors such as the severity and location of endometriosis, age, length of infertility and the presence of symptoms. And remember, while women with endometriosis are more likely to have fertility issues, only a small number of women will require IVF.
It is also important to remember to chat to your GP about your symptoms if you think you may have endometriosis.
If you end up going to hospital for surgery or a procedure, make sure you’re fully informed before you go. If you have private health insurance, it’s always a good idea to call them before you go – they can help you understand what your cover includes, what out-of-pocket costs you are likely to encounter and what you can expect from your hospital stay.
Endometriosis, fertility and pregnancy

-
What causes bad breath?
Find out how to keep your mouth smelling fresh
-
Signs to look out for when a cold is getting more serious
When you should see a doctor for a cold.
-
The health checks to keep in mind at different stages in your life
Have you had these health checks?
-
Bowel cancer: risks, symptoms, diagnosis and treatment
Learn more about bowel cancer
-
Flu myths debunked
Is 'man flu' real? Can you catch the flu from the flu vaccine? We separate flu facts from flu fictions.
-
Where to get health support in Australia
An Overseas Student Health Cover member’s guide to key health services and when to use them.
-
How can Australian pharmacies help you?
What can you buy at a pharmacy? Do you need a prescription? Can pharmacists identify health conditions? Everything international students need to know about pharmacies in Australia.
-
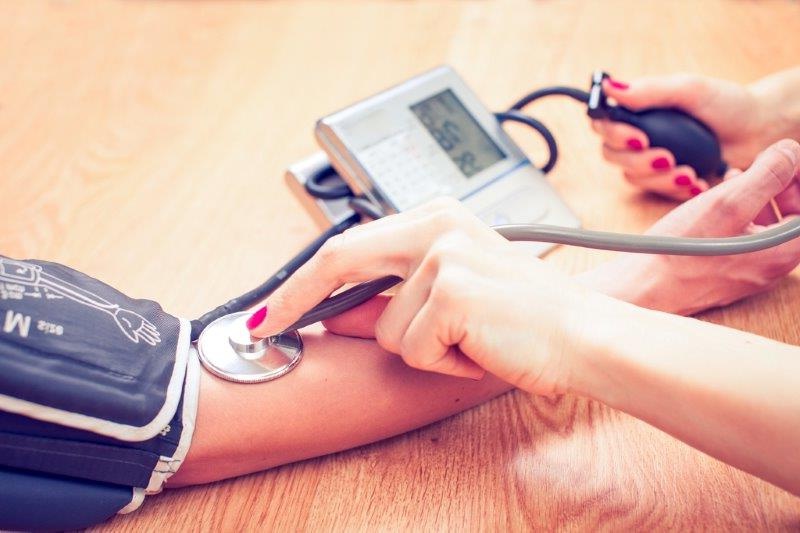
High blood pressure: how health cover can help
Put your health cover to use
-
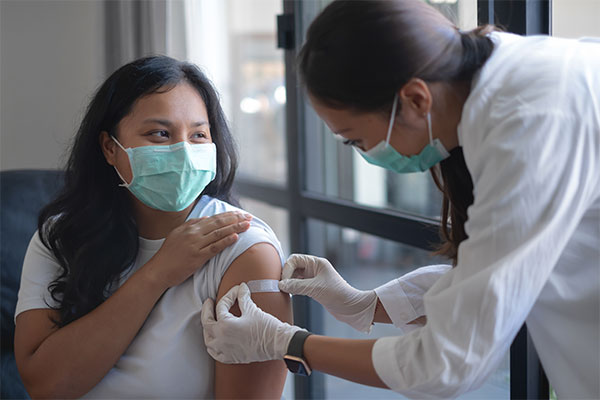
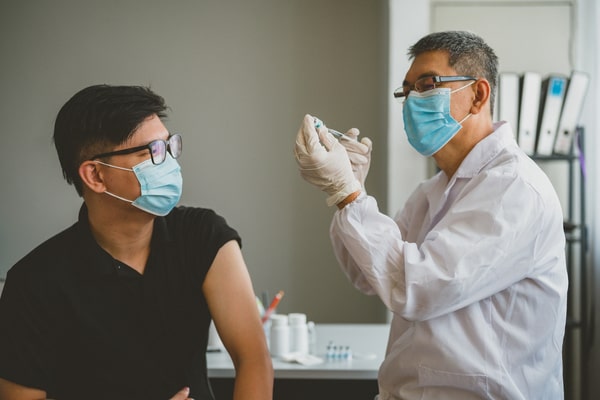
Why you should get the 2023 flu vaccine
More than three years on from the start of the COVID-19 pandemic, getting a flu jab this winter is even more important. Here’s why.
-
8 ways to prepare for cold and flu season
How to stay healthy this cold and flu season.
-
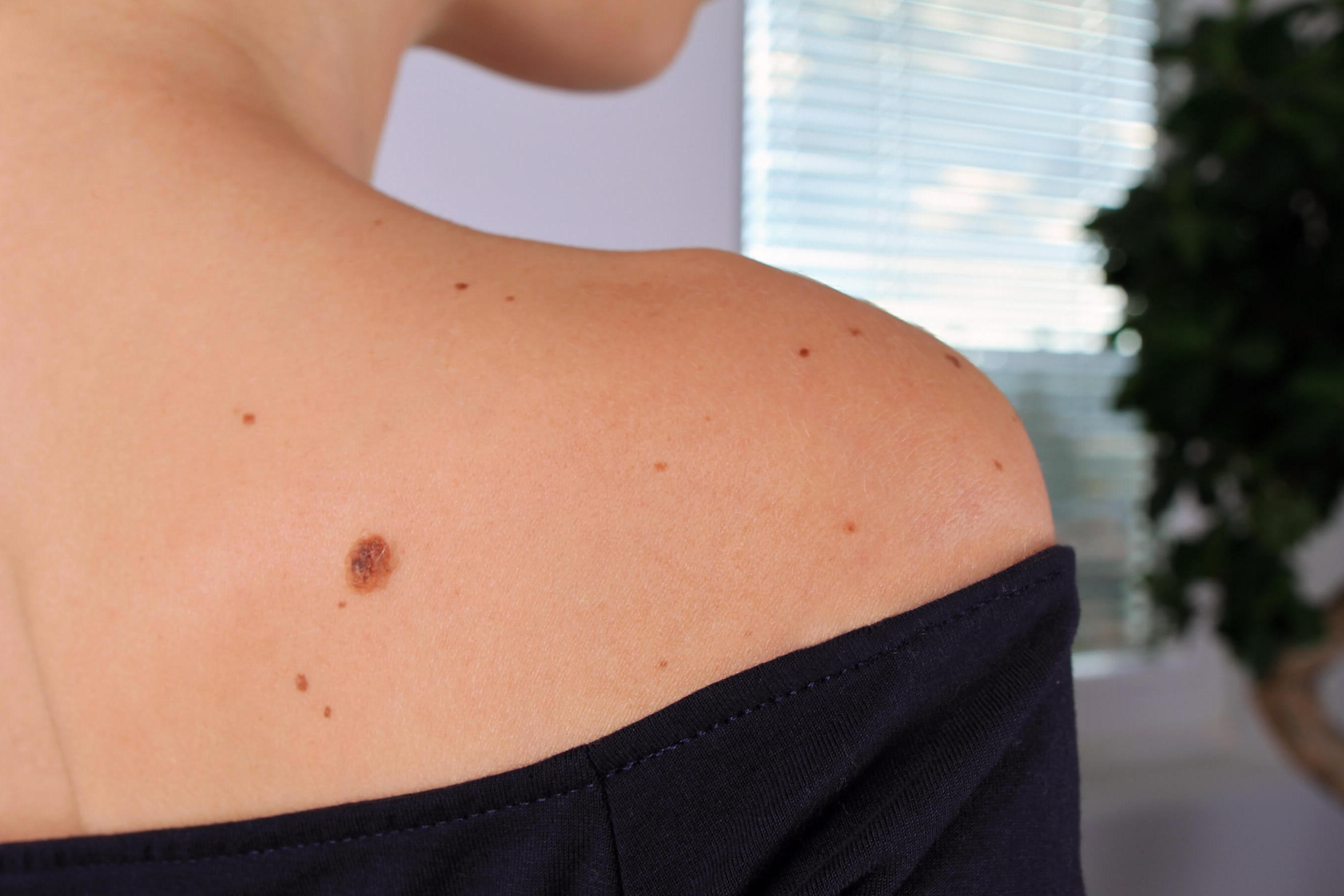
Spot the difference: Moles or melanomas?
A quick DIY skin check could save your life.
-
What is the 45-49 health assessment and am I eligible?
A government subsidised 45-49 year old health assessment can help Australians identify potential chronic conditions early and reduce the risks.
-
Health checks to help you stay healthy in your 40s
What health checks should you consider getting in your 40s and how often do you need them? Here’s your guide on how to stay healthy in your 40s.
-
Skin in the game
Let’s celebrate one of your body’s hardest workers - your skin.
-
Health checks by body part
We explore some common health checks, broken down by body part.
-
What cancer patients need to know about COVID-19
The COVID-19 pandemic might impact a cancer patient’s treatment. Here’s what you need to know, and how to look after yourself.
-
Have your kids had an eye check?
How often should kids get their eyes tested? What are the common signs of vision problems to look out for in children? We answer your questions here.
-
Your brain is a supercomputer
Humans are incredible, so we’re celebrating the extraordinary in what is often seen as ordinary, starting with the human brain.
-
Why it's time to check your blood pressure
You probably have a good idea what you weigh, how tall you are, or what your waist size is, but what about your blood pressure? Find out why it’s an important measure for you to know and keep an eye on.
-
Down, worried, or just feeling low?
Tips to manage your mental health.
-
How to guide teenagers through COVID-19
Beneath the poker face, your teenager may be feeling anxious about COVID-19 and going back to school. Here’s how you can guide them through it.
-
COVID-19 Vaccine boosters
COVID-19 booster vaccine shots; what do they do, who is eligible for it and where to book yours.
-
Patatas bravas recipe
Miguel Maestre, popular chef and co-host of The Living Room, shares his patatas bravas recipe.
-
5 healthy recipes for entertaining over the festive season
Indulge in the good things in life this holiday season, including these summer-inspired dishes.
-
Coping with change in the time of COVID-19
While the easing of COVID-19 restrictions has us knocking on the doors of loved ones and booking tables at our favourite restaurants, for some, the idea of life after lockdown and living with COVID-19 can be a little overwhelming. Here are some tips that may help.
-
OPSM shines light on link between mental health and eyesight
OPSM urges Australians to get their eyes tested this World Sight Day.
-
What to expect from a visit to the emergency department
Broken bones, snake bites and heart attacks are all reasons to go to an emergency department for urgent medical attention. Make sure you understand what to expect once you get there.
-
Chicken, lemon and dill soup recipe
Warm up with a soothing, comforting chicken soup.
-
Thai prawn fried rice recipe
Marion Grasby’s delicious recipe
-
COVID-19 vaccine rollout. What does it mean for international students?
Find out more about the COVID-19 vaccine in Australia, and when you might receive your COVID-19 vaccination.
-
Managing your blood pressure
Tips to manage your condition
-
COVID-19 vaccine rollout. What does it mean for you?
Find out more about the COVID-19 vaccine in Australia, and when you might receive your vaccination.
-
Does your child have a sleeping problem?
Recognise the signs and understand how to deal with them
-
Let's get behind the mask
Wearing a face mask during COVID-19: here are the guidelines.
-
Easy cheesy quiche recipe
Easy cheesy quiche recipe with variations
-
What causes muscle cramps?
And how to prevent them from cramping your style
-
Facing tough times with acceptance
The idea of acceptance is popping up everywhere from buddhism to the blogosphere, but how can we apply it to good effect in our lives?
-
A salute to our healthcare workers
Our healthcare workers have worked tirelessly to make sure that those who need it have support throughout these difficult times. Here we shine a light on the people who often don’t get the recognition they deserve.
-
How to balance your screen time during COVID-19
Give your eyes a break to avoid digital eye strain.
-
Telehealth explained
The coronavirus pandemic is changing the way we access our healthcare services – here’s what you need to know.
-
Physios warn of post-lockdown injury
Sports clubs and players are being urged to ensure they are match fit before they hit the court or field as coronavirus restrictions ease and sport resumes.
-
Our top COVID-19 apps
Social distancing, contact tracking and practising good hygiene have helped Australia flatten the curve, but new technology is going to keep us on top of it.
-
Diabetes and COVID-19
While this is a challenging time for all of us, people with diabetes may be feeling particularly vulnerable.
-
I suspect I have COVID-19. What next?
If you think you may have caught the novel coronavirus, here’s what you should do.
-
What to do if you have COVID-19
A guide to what you should do if you have COVID-19.
-
How to keep up with your health checks during COVID-19
How to see your doctor during COVID-19.
-
Is it safe to go to hospital during COVID-19?
What you can expect if you’re planning on going to hospital.
-
Everything you need to know about COVID-19
What it is, its symptoms, how it’s spread, who’s at risk, and how you can prevent it.
-
How to plan for a healthier future during COVID-19
Healthy changes that could have lasting effects.
-
Cancer and COVID-19: what you need to know
Tips to look after your physical and mental health.
-
Self-isolation: how it helps stop COVID-19 and tips to help you get through
Self-isolation: We're in this together, even if that means being alone.
-
How to talk about COVID-19 with your kids
Be prepared to answer the big questions from little ones.
-
The importance of having an asthma action plan
Are you or a loved one affected by asthma? You’re not alone.
-
What's the difference between paracetamol and ibuprofen?
Paracetamol vs ibuprofen
-
The difference between cold and flu
We explain the symptoms and best ways to recover
-
Bouncing back from the flu
Recovering from the flu? Here are our top tips to boost your health.
-
Inflammation: Friend or foe?
Understanding good and bad inflammation
-
Mushroom ragu: freezer friendly recipe
Try this freezer friendly mushroom ragu
-
What the wart?
Everything you’ve ever wanted to know about plantar warts
-
Recognising concussion in kids
Know when to seek help
-
How to deal with childhood food allergies
Don’t let food allergies hold your child back
-
Managing long-term lung problems (COPD): when to seek help
Know the signs of a flare up.
-
Managing long-term lung problems (COPD)
Tips to manage your condition.
-
Managing your heart disease
Tips to manage your heart disease
-
Spot the early warning signs of heart attack and stroke
Spot the signs
-
Post-traumatic stress disorder
Understand the symptoms and when to get help
-
Managing your health: your checklist
Are you managing your health as well as you could be?
-
Heart disease: how health cover can help
Heart disease? We might be able to help.
-
Prostate cancer: risks, symptoms, diagnosis and treatment
Learn more about prostate cancer
-
Managing your medications
Keep on top of your medications after hospital.
-
What does your tongue say about your health?
How to keep tabs on your tongue health
-
The kissing disease: How to deal with glandular fever
Why you get it and how to spot the symptoms
-
Do adults need to be vaccinated?
It may be time to get a booster
-
Is it time for a heart health check?
Taking one could save your life
-
Know the signs of a heart attack
With a heart attack, every minute counts
-
Anxious eaters anonymous
What causes us to overeat and how to combat it
-
Is arthritis affecting your mental health?
New Medibank data reveals you’re not alone
-
What does regular exercise do for your sex life?
We look at what the science says on sex and exercise.
-
Can you really break your penis?
The rumours are true - you can break your penis.
-
Acne: fact or fiction?
Is chocolate really to blame?
-
Cervical Screening: What do your results mean?
Our guide to interpreting your cervical screening results
-
Bowel cancer on the rise amongst young Aussies – could you be at risk?
Signs and symptoms of bowel cancer and how to prevent it
-
Caring for your hearing and your health
1 in 6 Australians experience some degree of hearing loss.
-
Keeping your kidneys healthy
How to prevent kidney disease
-
Why does my pee smell?
The smell of our pee can tell us a lot about our health.
-
What causes hiccups?
Stress and excitement are on the list
-
Why do we yawn?
Have you ever wondered why yawns are contagious?
-
Mental health support: who do I turn to?
Understand what your options are
-
What causes mouth ulcers?
Spoiler alert - stress is on the list
-
How alcohol affects your brain
Can a big night out really kill brain cells?
-
Is it time to see a lactation consultant?
Breastfeeding doesn't come naturally to everyone
-
Signs you might have an STI
And what you should do about it
-
Why you should call your grandparents more often
How social isolation affects physical and mental health
-
Shining a light on childhood cancer
Understand the signs and symptoms
-
Signs you might have a gambling problem
Use these checklists to see if you're at risk
-
What causes dandruff?
Can we do anything to prevent this head scratcher?
-
Should you worry about warts?
Most people will get one during their lifetime.
-
What causes depression?
Medibank mental health nurse Rachel Bowes explains
-
What causes low blood pressure?
Dr Linda Swan explains
-
What causes anxiety?
Medibank mental health nurse Rachel Bowes explains
-
What causes acne?
Find out whether junk food is to blame
-
How to manage panic attacks
Understand panic attacks, and how to prevent them
-
How to tell if your adult child is experiencing a mental health issue
Understand the signs of anxiety and depression
-
Brain cancer: risks, symptoms, diagnosis and treatment
Learn more about brain cancer
-
Understand psoriasis
How your misconceptions could be affecting sufferers
-
Butter or margarine?
We chew the fat to find out which one is better for you.
-
Bad cough? It could be whooping cough
Know the signs
-
Antibiotics: when do you really need them?
Our antibiotic use is amongst the highest in the world
-
The link between blood types and heart health
Could you be more at risk?
-
Not all headaches are created equal
Common headache types and what do about them
-
Suffering from a sore back?
Tips for preventing and managing back pain
-
Types of weight loss procedures
How do they work and who is suitable for them?
-
Common procedures explained: Colonoscopy
What to expect and how to prepare
-
Bowel cancer: Never too young
A young mother shares her story
-
Recovering from pacemaker surgery
What happens after you get home?
-
Preparing for pacemaker surgery
Give yourself the best chance of a quick recovery
-
Preparing for joint replacement surgery
Understand what to expect and prepare for your surgery
-
Tooth extractions explained
Learn more about common tooth extractions
-
Anxiety explained
Learn more about anxiety
-
Depression explained
Find out more about depression
-
Melanoma: risks, symptoms, diagnosis and treatment
Learn more about melanoma
-
Lung cancer: risks, symptoms, diagnosis and treatment
Learn more about lung cancer
-
Breast cancer: risks, symptoms, diagnosis and treatment
Learn more about breast cancer
-
Is your oral bacteria causing migraines?
A new study sheds some light
-
Who’s most at risk of loneliness?
And how you can alleviate symptoms
-
The physical effects of loneliness
Could loneliness be making you sick? We look at new research
-
What to do when Thunderstorm asthma strikes again
Advice from Epworth Respiratory Physician and Allergist, Dr Michael Sutherland
-
Thunderstorm asthma explained
How weather changes can trigger asthma symptoms
-
Asthma: why women need to take extra care
New data shows women over 55 are most at risk of dying from asthma
-
Osteoporosis and iron deficiency
Is there a link?
-
Recognising problem gambling
Only 15 per cent of problem gamblers ever seek help
-
Home from hospital: how to stay healthy
Steps to a strong recovery
-
Tips for your time in hospital
How to make your stay as comfortable as possible
-
Understanding hospital costs
Don’t be caught out by unexpected costs
-
Pumpkin and red lentil soup: freezer friendly recipe
A tasty variation of the classic
-
Life after cancer
For many people, a cancer journey doesn’t finish when their treatment ends
-
Does your child suffer from sleep apnoea?
The signs of sleep apnoea in kids
-
Mignonne’s experience with type 2 diabetes
See how one Aussie manages the condition
-
Managing a bowel cancer diagnosis
What to expect after diagnosis
-
A young runner and his journey with asthma
Watch 23 year old Aussie, Mathan, share his story
-
Living with anxiety
The various forms of anxiety and how they differ
-
Common heart procedures explained: coronary angiogram and coronary angioplasty
What you need to know about these common heart procedures
-
Killer heels
-
Cucumber and corn salsa recipe
Cucumber and corn salsa recipe
Subscribe to receive the best from Live Better every week. Healthy recipes, exercise tips and activities, offers and promotions – everything to help you eat, move and feel better.
By clicking sign up I understand and agree to Medibank's privacy policy