-
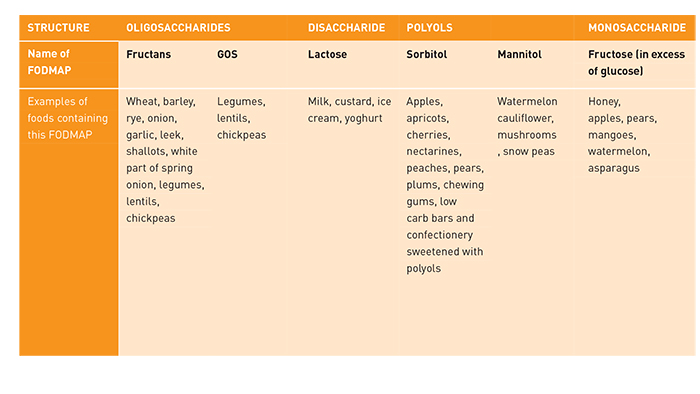
FODMAPs stands for Fermentable Oligosaccharides, Disaccharides, Monosaccharides and Polyols – a group of short-chain carbohydrates. These are found in a whole range of different foods, including garlic, onion, apples, milk, mushrooms, bread and chickpeas.
When these carbohydrates are poorly absorbed in the small intestine, increased water can be drawn into the gut. For some people this can result in diarrhoea, while for others, the carbohydrates travel to the large intestine where they are fermented by bacteria, producing gas.
This gas can lead to symptoms of Irritable Bowel Syndrome (IBS) including bloating, constipation, flatulence, pain and nausea.
The concept of FODMAPs was first developed by Advanced Accredited Practising Dietitian Dr Sue Shepherd in 2005. Since then, the research team at Monash University has been leading the way in research relating to IBS and the role that FODMAPs play in symptoms.
Understanding FODMAPS and IBS

-
"Research shows that following a low FODMAP diet is the most effective way of managing IBS, with three in four people finding an improvement in symptoms."
Who needs to worry about FODMAPs and why?
At present, around one in seven Australians suffer from this difficult condition. It is a chronic condition, meaning long term management is required, though symptoms and severity often change over time.
IBS can be defined through symptoms of cramping, abdominal pain, bloating, flatulence, constipation and diarrhoea. These symptoms can often worsen in times of stress.
Research shows that following a low FODMAP diet is the most effective way of managing IBS, with three in four people finding an improvement in symptoms.
What is the process?
By reducing consumption of high FODMAP foods, symptoms of IBS can clear up in a matter of weeks.
However, a strict low FODMAP diet is a diagnostic tool – it is not recommended to be followed long term. Once it has been determined that FODMAPs are causing grief, moving through a series of food challenges is essential to help determine which particular FODMAPs are an individual’s triggers.
Why not just stay low FODMAP?
Most people’s symptoms are only triggered by a few of the high FODMAP groups of foods. Identifying these means you can reintroduce the groups of foods that don’t cause a problem, and determine tolerance levels of those that do. This is recommended for the following reasons:
- Most people with IBS can maintain good symptom control with the reintroduction of some high FODMAP foods. This makes it easier to make informed choices and better manage symptoms on a daily basis.
- Avoiding unnecessary restrictions helps ensure a nutritionally adequate diet.
- Many high FODMAP foods are also high in prebiotics. These provide food for the healthy bacteria that are found in your gut. Long term avoidance of these may affect the health of your microbiome.
What if a low FODMAP diet doesn’t work?
Other things can trigger symptoms of IBS. These include fatty foods, spicy foods and caffeine. Stress also plays a key role in symptom management, so managing stress levels regularly helps with reducing symptoms.
-
How is ‘phubbing’ hurting your relationships?
Here’s how to stop phubbing and be more mindful of your phone habits, to help improve face to face interactions with your family and friends.
-
Are the winter blues real?
Simple ways to boost your mood in winter.
-
Mental fitness explained
Just as you work to strengthen your body, your mental health deserves attention and exercise too.
-
Signs it's time to visit the dentist
Nobody wants to go. But there are good reasons to – promise.
-
The link between stress, anxiety and jaw pain
Physiotherapist Michael Chan explains how stress and anxiety can cause jaw pain, and how to help get some relief.
-
When you can't sleep next to your partner
You love everything about them – except their sleep habits.
Subscribe to receive the best from Live Better every week. Healthy recipes, exercise tips and activities, offers and promotions – everything to help you eat, move and feel better.
By clicking sign up I understand and agree to Medibank's privacy policy





.jpg)
